Vasopressor use in Septic Patients: New Paper Highlights Limitations of Hemodynamic Monitors that Derive Blood Flow Solely from Pressure
Vasopressor Implications Explored
A new clinical paper investigates therapeutic approaches, specifically vasopressor use, in septic patients. The study emphasizes the need for hemodynamic monitoring that uses a technique that is independent of blood pressure.
Published in the European Journal of Anaesthesia (EJA), June 21 and authored by Feldheiser et al, the paper is titled; “Vasopressor effects on venous return in septic patients: a review.
The authors describe this manuscript as being based on a literature search in PubMed, coupled with their own research activities in the field. It is accompanied by an interview with the author.
Cardiac Output Monitoring Recommendation
The authors emphasize the importance of monitoring cardiac output using blood-pressure-independent methodology. This is because systems that use blood pressure as an indirect, surrogate indicator of hemodynamic status cannot provide the vital picture of vasopressor impact on venous return and, by extension the microcirculation.
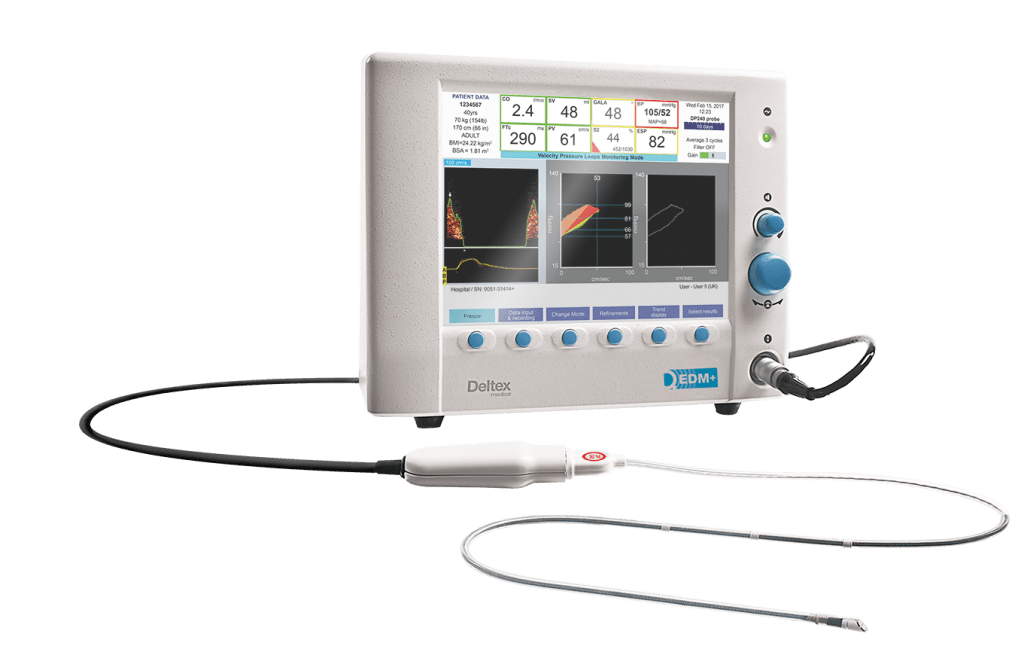
TrueVue EDM+ (pictured) measures real-time, accurate cardiac output, directly from the patient’s aorta.
Hemodynamic Management of the Septic Patient when Vasopressor Therapy is Employed
Fluid resuscitation in septic patients is a key element of the initial therapy. If fluid therapy fails to stabilize the hemodynamics, septic shock can ensue. At this point clinicians employ vasopressor therapy to maintain organ perfusion pressure.
Norepinephrine is the first choice vasopressor, as recommended in surviving sepsis campaign guidelines. After reviewing the range of alternative vasopressors, Feldheiser et al go on to talk about the secondary effects of vasopressor therapy beyond the desirable increase in arterial pressure. In particular they discuss the venous component of the circulatory system.
The author elegantly explains what is a fascinating, yet complicated picture: While vasopressor therapy typically brings about vasoconstriction, this can be accompanied by a corresponding reduction in venous return in septic patients. Importantly from a therapeutic perspective, not all vasopressors increase tone in post-capillary venules. This can lead to edema, flow problems and reduced venous return.
“Hypotension is not a single sign of low arterial blood pressure (ABP). It is an expression of physiological disregulation leading to, at one point, low ABP. There are many underlying background pathophysiological issues that have to be considered.” Aarne Feldheiser
Three take-homes
Undesirable impacts on the microcirculation can occur in the face of apparently successful mean arterial pressure therapy. Indeed events occurring in the microcirculation can actually undermine efforts to restore hemodynamic balance. In the accompanying podcast, Dr Feldheiser offers up three take-home messages:
- Firstly, the interaction between cardiac output and arterial tone: If the clinician increases vasopressor only to see a decrease in cardiac output, Feldheiser says “please consider your alternatives” because this could well be symptomatic of fluid accumulation in the venous system.
- Secondly, to reinforce the point, Dr Feldheiser talks of a study in sepsis patients in which he used doppler monitoring (Deltex EDM+) to measure stroke volume. Researchers saw temporary increases following subsequent fluid applications. This unsustained increase in stroke volume is symptomatic of problems in venous return. His conclusion is that appropriate therapy is about more than simply fluid and in particular fluid responsiveness.
- Thirdly, based on these pillars, he suggests that future monitoring should include a more holistic approach to the circulation and should always include Cardiac Output.
“We propose that future research includes the measurement of cardiac output by a blood-pressure-independent methodology to assess a possible impact on venous return, a cardiac performance variable to avoid the negative impact of an increase in afterload, and if possible, a marker of microperfusion for evaluating vasopressor response.” Aarne Feldheiser
Deltex comments
Andy Mears, Deltex CEO comments: “The authors clearly recognize the need for advanced hemodynamic information that is independent of blood pressure. They refer to ‘filling the black box of septic patients with light’. This means having the most complete picture of the full impact of circulatory interventions to guide clinical decisions. At Deltex we’re firmly supportive of the need to have the best possible window into the patient’s hemodynamic status. Indeed our TrueVue EDM+ system provides real-time, accurate cardiac output data directly from the aorta and can combine these readings with independently measured blood pressure. The perfect solution!”





